Jun 16, 2022
To Achieve Health Equity, Build a “Coalition of Coalitions”
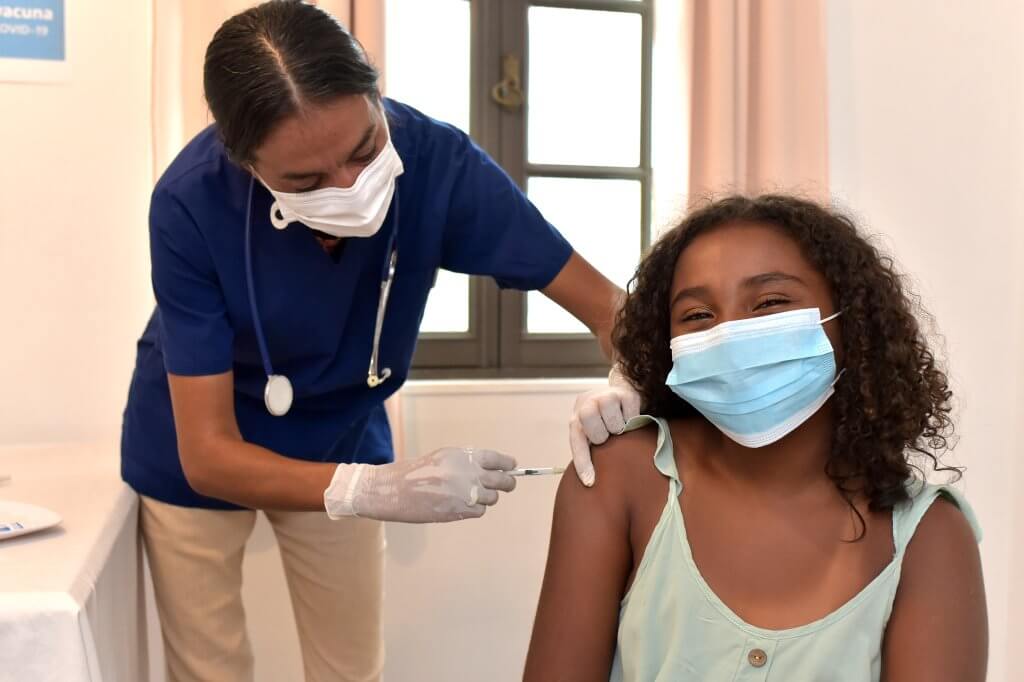
Nurses’ efforts to achieve health equity are always stronger when they form partnerships with the community being served. That’s why matching funding and local partnerships were a requirement for every project supported by the Future of Nursing: Campaign for Action’s Nursing Innovations Fund. The connections facilitated by this design were essential for these projects’ impact.
But an Innovation awardee in North Carolina took an especially effective approach to forming partnerships: engaging a “coalition of coalitions.”
This approach was pursued by Project RARE (Reciprocal, Authentic Relationships for Equity), an initiative of the North Carolina Agricultural and Technical University (NC A&T) supported by the North Carolina Action Coalition, a state-based arm of the Campaign. Initially focused on COVID-19 vaccinations in underserved communities, the program has since expanded to focus on an array of health conditions in African-American and rural communities.
According to program leaders, the relationships at the heart of this initiative were actually formed at a meeting about the Campaign’s Health Equity Toolkit. That’s where the Campaign, an initiative of AARP Foundation, AARP and the Robert Wood Johnson Foundation, took care to introduce Action Coalition leaders with representatives of Historically Black Colleges and Universities (HBCUs) from their states. That’s how Valerie Howard, EdD, RN, FAAN, met Lenora Campbell, PhD, RN.
“That was where the relationship began,” said Howard, who was recently named Dean of the College of Nursing at University of North Carolina Chapel Hill. “It’s all about building and maintaining relationships with others, even if you don’t know exactly what opportunity is going to come of that.”
Howard and Campbell, who served as Dean of NC A&T’s College of Health and Human Sciences until 2021, were soon using the toolkit to design a new approach to addressing social determinants of health in North Carolina. Cone Health, their partner and the provider of the matching funds, identified six North Carolina ZIP Codes with the highest number of low-acuity emergency room visits — a classic sign that a community lacks access to health care resources.
Then the team worked with churches in each ZIP Code to identify their most important health needs. Crucial to this partnership was the Congregational Nurse Program established by Cone Health in 1998, which had already identified trusted health professionals in many faith communities.
Congregational nurses are members of churches who serve as health advisers to their co-parishioners. According to Howard, these members of the most trusted profession enjoy an even higher level of trust. “It’s not just that you brought in a nurse to speak to this congregation,” she said. “She is a part of the congregation, a trusted member of the community.”
By the time Howard and Campbell began meeting with the pastors and nurses, it was clear that the COVID-19 pandemic would be the most pressing health need for their communities. So they agreed to work with Cone Health and the Guilford County Health Department to set up church-based sites for testing and vaccinations.
Campbell said that an important strength of the churches, Cone Health, and all the partners involved in the work was that they each already represented strong local coalitions. This helped bring whole communities on board from the start.
“If you can come to the table with people who already understand the importance of forming partnerships and coalitions, and who bring some themselves, then you are going to be ahead of the game,” Campbell said.
“You can already have diversity of thought when you receive an opportunity,” Howard added. “We all bring our own ideas and opinions, and that strengthens any proposal or initiative.”
That’s not to say the program did not face challenges, however. Campbell said that in early conversations, it was unclear what role pastors would play. They were more comfortable serving as spiritual leaders than health leaders, she said.
“They were pretty quiet in those meetings when we started out,” she said. “We let them be quiet if that is what they needed to be. But then we provided expertise that helped them feel like they could engage on these issues.”
One key area where the pastors could lead was building trust. As in underserved communities all over the country, the mostly Black church communities had a higher level of distrust in the health care system due to a history of racial violence and oppression.
The team took care to explicitly address these concerns. For example, presentations by a virologist explicitly contrasted the development of today’s vaccines with traumatic episodes from the past such as the Tuskegee Syphilis Study.
“He couched what he was saying in terms of historical information for marginalized communities,” Campbell said. “For many of the pastors, this was an a-ha moment. It said ‘We have this history, but we also have this virus that knows no history.’ The virologist himself was African-American, so he understood the full weight of what they were dealing with.” The pastors, in turn, felt comfortable embracing the information shared.”
While the counties targeted by the program had COVID-19 vaccination rates that were lower than average overall, the data show signs of hope in the communities being served by the program, with vaccination rates rising among the targeted communities The team attributes this difference to the work of Project RARE.
Now the project has turned to designing interventions for hypertension, cardiovascular disease, and other chronic diseases exacerbated by social determinants of health. But no matter what health issues are addressed, Campbell said, nurses will still be key to the program’s success.
“Nurses have always been focused on the whole patient,” she said. “That’s our history. They were focused on social determinants before anyone even coined the term.”
If you want to build programs like the one that emerged in North Carolina, learn more by visiting the Nursing Innovations Fund page or by downloading the Campaign’s Health Equity Toolkit.
